what can you say to someone that has an incurable disease
 The Pew Research survey asked respondents nigh their personal preferences for medical treatment in different scenarios. A bulk of adults (57%) say they would enquire their doctors to finish medical treatment if they had a disease with no hope of improvement and they were suffering a not bad deal of pain, while 35% would tell their doctors to do everything possible to salvage their lives in such a state of affairs.
The Pew Research survey asked respondents nigh their personal preferences for medical treatment in different scenarios. A bulk of adults (57%) say they would enquire their doctors to finish medical treatment if they had a disease with no hope of improvement and they were suffering a not bad deal of pain, while 35% would tell their doctors to do everything possible to salvage their lives in such a state of affairs.
Nigh half of adults (52%) say they would desire to stop handling if they had an illness or condition that made them totally dependent on another person for their intendance, while 37% say they would want to do everything possible to save their lives in this situation.
Preferences are evenly divided when information technology comes to an incurable illness or status that makes it difficult to part in twenty-four hours-to-solar day activities: 46% say they would opt to finish medical handling, and an equal share say they would desire their doctors to do everything possible to salve their lives in that circumstance.
Personal preferences nigh end-of-life medical treatment take inverse modestly over time. Compared with 1990, a somewhat greater share of the public today expresses a preference on each of these questions; in addition, a somewhat greater share of adults today say they would tell their doctors to practice everything possible to relieve their lives if faced with an incurable illness. The share of Americans who say they would tell their doctors to stop their handling and so they could dice remains about the same as in 1990.
 To what extent are public preferences well-nigh stop-of-life medical treatment consequent across circumstances? Well-nigh a third of U.Due south. adults (32%) say they would stop their treatment in all three of the circumstances included in the survey, a fifth (20%) would ask their doctors to do everything possible to save their lives in all three circumstances, and 46% have varying preferences depending on the exact circumstances.
To what extent are public preferences well-nigh stop-of-life medical treatment consequent across circumstances? Well-nigh a third of U.Due south. adults (32%) say they would stop their treatment in all three of the circumstances included in the survey, a fifth (20%) would ask their doctors to do everything possible to save their lives in all three circumstances, and 46% have varying preferences depending on the exact circumstances.
The share of Americans who consistently say they, personally, would cease their treatment so they could die in all three of these cases is roughly the same as it was in 1990 (32% today vs. thirty% in 1990). Compared with a 1990 Pew Research survey, more adults today say they would tell their doctors to practice everything possible to relieve their lives (upwards 6 percentage points) and fewer have varied preferences depending on the circumstances considered (downwardly 7 percentage points since 1990).

Personal preferences about end-of-life medical treatment are strongly related to age and to race or ethnicity.
For instance, adults ages 50 and older are more inclined to say they would end their treatment so they can dice in all three cases considered. Roughly four-in-ten adults ages l-64 (43%) say this for all three questions, equally do like shares of those ages 65-74 (42%) and those ages 75 and older (41%). By comparing, 23% of adults under age fifty say they would want to stop their treatment in all 3 circumstances.
In terms of race and ethnicity, blacks and Hispanics are more likely than whites to say they would tell their doctors to do everything possible to save their lives in all three situations; four-in-x blacks (xl%) and virtually a third of Hispanics (32%) say this, compared with 14% of non-Hispanic whites. Past comparison, whites are more inclined to say they would end their medical handling in all three circumstances (35%).
Differences among religious groups are more than modest and are largely in keeping with differences by race and ethnicity on this summary measure. On the one hand, most a third of white evangelical Protestants (33%), white mainline Protestants (33%) and white Catholics (35%) say they would finish their medical handling in all iii situations. A similar share of the religiously unaffiliated say the aforementioned (38%). On the other hand, blackness Protestants and Hispanic Catholics are more probable to say they would tell their doctors to do everything possible to save their lives in all three cases (42% and 33%, respectively). Amid white mainline Protestants, 57% accept preferences for medical handling that vary depending on the circumstances.
Americans who have given a neat deal of thought to their own wishes most end-of-life treatment are more inclined to say they would want to stop their treatment so they could dice in all three cases (38%, compared with 23% among those who have given piddling or no thought to their wishes). Past contrast, personal preferences most stop-of-life treatment are not significantly related to having had a shut friend or relative with a concluding illness in contempo years. And there is non much deviation in personal preference well-nigh end-of-life medical handling based on a person's own electric current wellness status.
Attending to and Experience With End-of-Life Treatment
 The corporeality of idea and attention U.South. adults give to end-of-life issues varies; 37% of adults study having thought "a great deal" about end-of-life handling prior to taking the survey. Another 35% say they have given "some" idea to these issues and 27% have given "non very much" or no prior idea to their terminate-of-life preferences.
The corporeality of idea and attention U.South. adults give to end-of-life issues varies; 37% of adults study having thought "a great deal" about end-of-life handling prior to taking the survey. Another 35% say they have given "some" idea to these issues and 27% have given "non very much" or no prior idea to their terminate-of-life preferences.
The share of Americans who say they take given their own wishes near end-of-life handling a great deal of idea is about the same equally in the 2005 survey and up 9 percentage points since 1990 (when it stood at 28%).
Last illness has touched the lives of many U.S. adults, 47% of whom take recent personal feel with a close friend or family fellow member suffering from this type of illness. Nigh half of those with such a friend or family unit member (23% of all adults) report that the effect of withholding life-sustaining handling arose for that person. Since 2005, feel with a close friend or relative facing a terminal illness is up 5 pct points.
As expected, feel with a close friend or relative facing a final illness cuts across social and demographic groups, including age, gender, didactics and religious groups. For example, 46% of adults ages 18-49 say a close friend or relative has had a terminal illness or been in a coma within the past five years, and 48% of adults ages 50 and older say the same. However, fewer Hispanics than whites (36% and fifty%, respectively) have had a loved one in this situation; amongst blacks the comparable figure is 45%.

 Not surprisingly, experience with a friend or relative facing a serious illness is associated with more attention to one'due south own wishes about end-of-life care; 45% of those with a terminally sick friend or relative say they accept given a great deal of thought to their ain wishes, compared with 31% of those without this kind of close experience.
Not surprisingly, experience with a friend or relative facing a serious illness is associated with more attention to one'due south own wishes about end-of-life care; 45% of those with a terminally sick friend or relative say they accept given a great deal of thought to their ain wishes, compared with 31% of those without this kind of close experience.
Thinking about one'due south own wishes as well is related to a respondent'south historic period and personal health.
Amidst adults ages 75 and older, 47% study having given a great deal of thought to their own wishes about end-of-life treatment. By contrast, most a third (32%) of adults ages xviii-49 say the same.
Those who describe their current wellness as fair or poor (of whom roughly one-half are ages l and older) are more likely to have given a great bargain of thought to their wishes for finish-of-life treatment (47%) compared with those who say their health is good (33%) or excellent (36%).
There are no or simply modest differences in the corporeality of thought given to one'due south end-of-life wishes by gender, race and ethnicity. Nor are there significant differences in the likelihood of having given end-of-life issues a great bargain of thought by pedagogy, religious amalgamation or frequency of worship service attendance.
Communicating I's Wishes About Stop-of-Life Handling
Pew Research surveys from 1990, 2005 and 2013 show that a majority of adults say they take talked with someone else about their wishes regarding stop-of-life treatment, but substantially fewer have written downwardly these thoughts.
 The 2013 survey finds that 35% of adults say they have their wishes in writing or that they take a living will. This is roughly the same share equally in 2005 (34%) simply upward essentially from ane-in-half-dozen adults (16%) in 1990.ix
The 2013 survey finds that 35% of adults say they have their wishes in writing or that they take a living will. This is roughly the same share equally in 2005 (34%) simply upward essentially from ane-in-half-dozen adults (16%) in 1990.ix
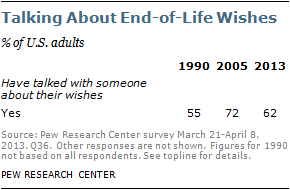 Past comparison, having talked with someone else near end-of-life handling preferences is more than mutual. A majority of Americans say they have done so, as was the case in 1990 and 2005. But these figures have fluctuated some over the years. Today, roughly vi-in-ten adults (62%) say they take talked with someone else most their wishes, downwardly from 72% in 2005 simply upwards modestly from 55% in 1990.10
Past comparison, having talked with someone else near end-of-life handling preferences is more than mutual. A majority of Americans say they have done so, as was the case in 1990 and 2005. But these figures have fluctuated some over the years. Today, roughly vi-in-ten adults (62%) say they take talked with someone else most their wishes, downwardly from 72% in 2005 simply upwards modestly from 55% in 1990.10
 Altogether, about 2-thirds of the general public has taken some sort of activity to communicate their wishes for end-of-life intendance. A third of adults (33%) accept neither talked about their wishes with others nor written their wishes downwards.
Altogether, about 2-thirds of the general public has taken some sort of activity to communicate their wishes for end-of-life intendance. A third of adults (33%) accept neither talked about their wishes with others nor written their wishes downwards.
Not surprisingly, younger adults, particularly those nether historic period 30, are less probable to have communicated their wishes about end-of-life treatment. Just 15% of immature adults ages 18-29 say they take their wishes near finish-of-life care written down. By dissimilarity, half dozen-in-ten adults ages 65 and older have their wishes in writing.
Differences past historic period are still apparent, fifty-fifty if not as stark, when factoring in both talking about and writing down i's wishes for end-of-life treatment. Nigh half of adults under age 30 say they have either talked about or written downwardly their wishes (48%), compared with three-quarters of those ages 75 and older.
More than whites (74%) than blacks (49%) and Hispanics (l%) have communicated their end-of-life wishes either verbally or in writing. In addition, Americans with more years of formal didactics are more likely than those with less teaching to have written downwards or talked with someone about their end-of-life wishes, and those with higher incomes are more probable than lower-income adults to say they have washed this. And, not surprisingly, the amount of prior thought people take given to the issue too is correlated with whether they accept talked about or written downward their wishes. By contrast, respondents' personal health status is not significantly related to whether or not they have communicated their finish-of-life wishes either verbally or in writing.
Source: https://www.pewresearch.org/religion/2013/11/21/chapter-3-personal-wishes-for-and-attention-to-end-of-life-treatment/
0 Response to "what can you say to someone that has an incurable disease"
Post a Comment